|
Īs smaller pulmonary emboli tend to lodge in more peripheral areas without collateral circulation, they are more likely to cause lung infarction and small effusions (both of which are painful), but not hypoxia, dyspnea, or hemodynamic instability such as tachycardia. A low-grade fever may be present, particularly if there is associated pulmonary hemorrhage or infarction. Strain on the right ventricle may be detected as a left parasternal heave, a loud pulmonary component of the second heart sound, and/or raised jugular venous pressure. A pleural effusion is sometimes present that is exudative, detectable by decreased percussion note, audible breath sounds, and vocal resonance. Occasionally, a pleural friction rub may be audible over the affected area of the lung (mostly in PE with infarct). On physical examination, the lungs are usually normal. 
While PE may present with syncope, less than 1% of syncope cases are due to PE. About 15% of all cases of sudden death are attributable to PE. More severe cases can include signs such as cyanosis (blue discoloration, usually of the lips and fingers), collapse, and circulatory instability because of decreased blood flow through the lungs and into the left side of the heart. Symptoms of pulmonary embolism are typically sudden in onset and may include one or many of the following: dyspnea (shortness of breath), tachypnea (rapid breathing), chest pain of a "pleuritic" nature (worsened by breathing), cough and hemoptysis (coughing up blood). They become more common as people get older. In the United States, between 300,000 and 600,000 cases occur each year, which contribute to at least 40,000 deaths. Pulmonary emboli affect about 430,000 people each year in Europe. If blood thinners are not appropriate, a temporary vena cava filter may be used. Severe cases may require thrombolysis using medication such as tissue plasminogen activator (tPA) given intravenously or through a catheter, and some may require surgery (a pulmonary thrombectomy). However, treatment using anticoagulants is not recommended for those at high risk of bleeding, as well as those with renal failure. These are recommended for at least three months. Treatment is with anticoagulants such as heparin, warfarin or one of the direct-acting oral anticoagulants (DOACs). Įfforts to prevent PE include beginning to move as soon as possible after surgery, lower leg exercises during periods of sitting, and the use of blood thinners after some types of surgery. Together, deep vein thrombosis and PE are known as venous thromboembolism (VTE). Otherwise, a CT pulmonary angiography, lung ventilation/perfusion scan, or ultrasound of the legs may confirm the diagnosis. If the risk is low, a blood test known as a D-dimer may rule out the condition. Diagnosis is based on signs and symptoms in combination with test results. A small proportion of cases are due to the embolization of air, fat, or amniotic fluid. The risk of blood clots is increased by advanced age, cancer, prolonged bed rest and immobilization, smoking, stroke, long-haul travel over 4 hours, certain genetic conditions, estrogen-based medication, pregnancy, obesity, trauma or bone fracture, and after some types of surgery. PE usually results from a blood clot in the leg that travels to the lung. Severe cases can lead to passing out, abnormally low blood pressure, obstructive shock, and sudden death. Signs of a PE include low blood oxygen levels, rapid breathing, rapid heart rate, and sometimes a mild fever. 
Symptoms of a blood clot in the leg may also be present, such as a red, warm, swollen, and painful leg. Symptoms of a PE may include shortness of breath, chest pain particularly upon breathing in, and coughing up blood. 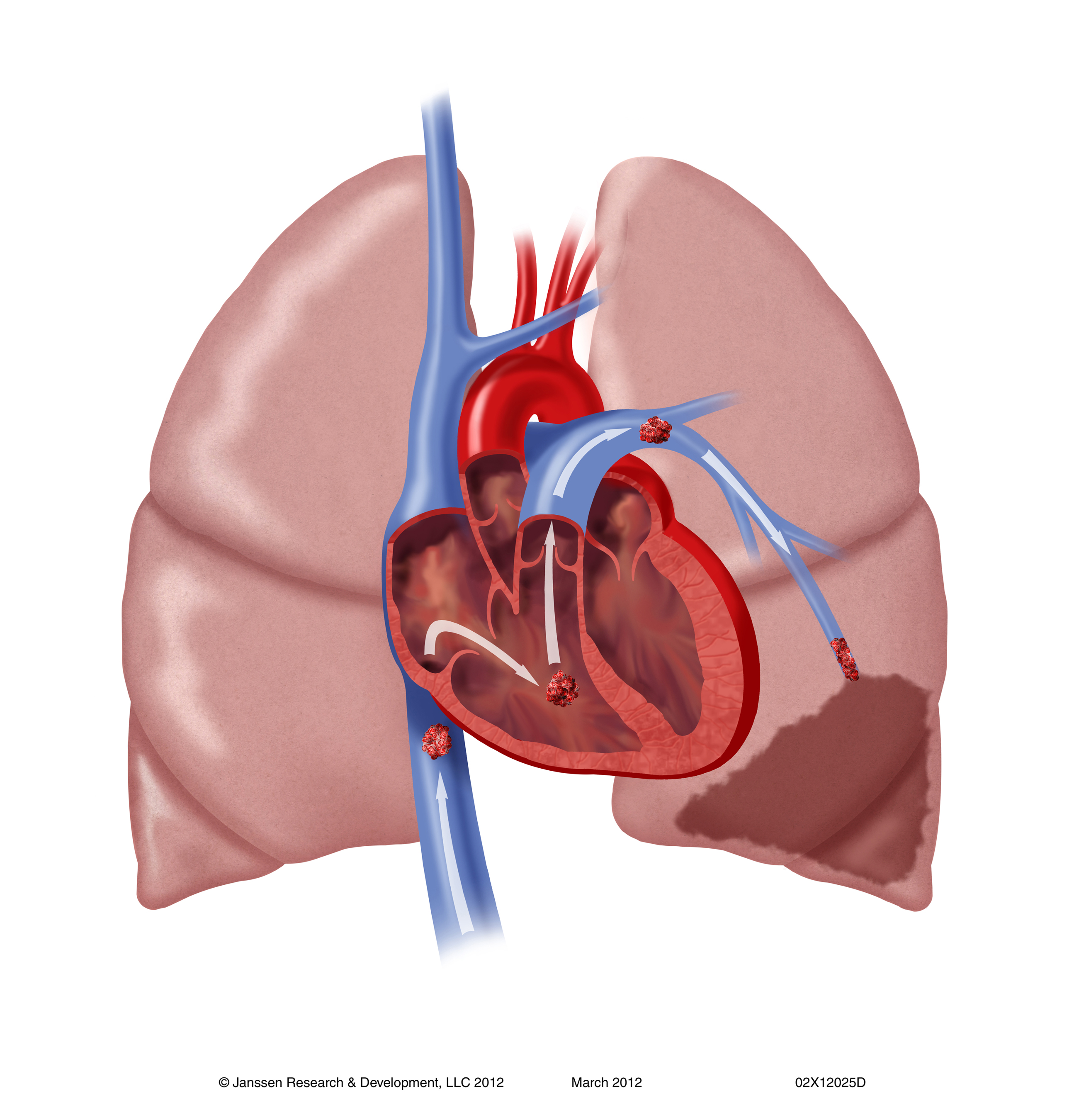
Pulmonary embolism ( PE) is a blockage of an artery in the lungs by a substance that has moved from elsewhere in the body through the bloodstream ( embolism). Passing out, abnormally low blood pressure, sudden death chronic thromboembolic pulmonary hypertension (long-term complication)Ĭancer, prolonged bed rest, blunt trauma, smoking, stroke, certain genetic conditions, estrogen-based medication, pregnancy, obesity, after surgery īased on symptoms, D-dimer, CT pulmonary angiography, lung ventilation/perfusion scan Īnticoagulants ( heparin, warfarin, DOACs) 
Shortness of breath, chest pain, coughing up blood A lung illustration depicting a pulmonary embolism as a thrombus (blood clot) that has travelled from another region of the body, causes occlusion of the pulmonary bronchial artery, leading to arterial thrombosis of the superior and inferior lobes in the left lung
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
